Stress & health professionals – Ten coping strategies
It was three years ago and I was operating on a 75 years old male with multiple medical problems who had a major acute and chronic gallbladder disease and needed urgent gallbladder removal. I was preoccupied with number of his medical issues and the difficulty of his surgery when a branch of cystic artery started to bleed profusely. My heart was racing. I tried to use the clip applier to clip the artery but the clip got jammed in the device and wasn’t functioning anymore. I asked the circulating nurse to give me another one, but there was no clip applier in the room and she had to run out to get a new one. I experienced extreme fear, fear of inability to control the bleeding and losing my patient. My heart rate was soaring. I put pressure on the artery to slow down the bleeding until she came back into the room. It probably took thirty seconds but for me it felt like days. There was a puddle of blood in the area of gallbladder and I couldn’t see the artery, so I placed the suction device to suction the blood, but suction was not connected. I called her again to connect the suction but it wasn’t functioning and she had to go out to bring another one into the room. I got extremely angry and my heart was pumping harder and harder. It took probably another sixty seconds for the suction to work, but for me it felt like eternity. For a few seconds I experienced tightness in my chest. I could even feel my coronary arteries going into spasm. I experienced an array of negative emotions of fear, anger and disappointment which made me feel miserable. But, I had to save that patient regardless of how dispirit I felt. So I shouted my name to redirect my full attention to the bleeding (that’s what I usually do in the crazy situations), kept the pressure on the artery and took a couple of deep breaths to calm down my heart. Now the suction was working and the clip applier was firing and the bleeding was stopped. My patient did very well after the operation and did not require any transfusion and went home on the following day.
I’m sure you probably have many stories of stressful events and struggles at work. Some of you may refer to them as:
Oh my god, I have too many tasks to do. There is so much paperwork to fill out. I feel like I`m behind the computer all day! I have too many patients to take care of. I can’t stand that arrogant doctor who walks around and screams at me every time he comes to the floor. It’s so hard to work with that nurse, it seems like she doesn’t know much or maybe she doesn’t even want to do anything. I have a difficult patient. Those family members are so demanding. For what I do every day I don’t get enough salary and benefit. I can`t work with my supervisor, she is so pushy, bossy and unappreciative. The emotional roller-coaster in my daily work is too much to tolerate.
These are just some of the daily struggles and stress in the health care workplace and without a doubt there are many more. Medical profession is very unique in this respect. We are dealing with people’s life, their pain, medical problems, psycho-social issues and dispirit family members. It automatically creates a stressful environment and then on top of that the demanding health care system, its new rules, regulations and expectations, has intensified the pressure of the workplace. The chronic presence of these stressors at work not only has been associated with so many individual health consequences but it also has created a culture of indifference in our workplace and made it more unpleasant and stressful. It has also increased the risk of medical errors, decreased the productivity of the health professionals and reduced the patient satisfaction.
Ten Coping Strategies on how to deal with stress
The idea is not to decrease or avoid these stresses, because it usually wouldn’t work, but to find the ways to cope with these stressful situations. Before we talk about the strategies of coping with stress, let`s define the stress and see how it affects our mind and our body.
The stress is an individual perception of a physical, mental or emotional stimulus as a challenging, threatening or overwhelming event when it exceeds our available coping resources. It starts with an event or stimulus which is sensed, processed and appraised in our brain and then activates a biological response, called stress response. The characteristics of the individuals, their priorities, experiences, goals, values, beliefs, and their physical and psychosocial resources for coping, make a huge difference in how stressful a situation may be perceived.
Stress response is an innate and adaptive response in our body which alerts and protects us against any harmful situations. It allows us to focus our mental and physical resources to deal with the stressful events. The stress response increases our energy and immunity, focuses our attention, improves our working memory and cognitive ability and enhances our performance. However, when the stressful events are extreme, continuous or repetitious they may be harmful and lead to stress-related disorders.
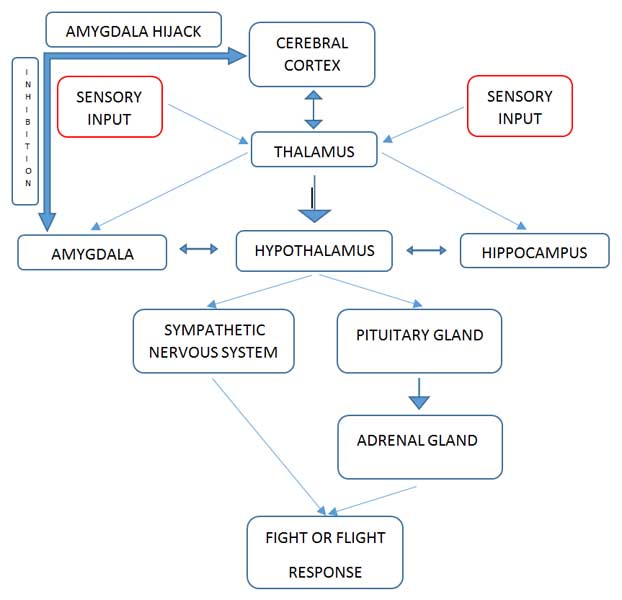
Over last two decades, numerous neurobiological studies have shown the extremely complex circuits in our brain accountable for this response. When the stressful stimulus is perceived through our senses, it activates the amygdala. Amygdala is a part of the limbic system which is essential in our emotional life and memories for emotional events. Amygdala is heavily involved in fear cascade but it is also linked in other emotional responses. If the stimulus is perceived as harmful or threatening, it will activate a neuroendocrine cascade through the hypothalamus-pituitary-adrenal axis and initiate the so called “fight or flight response”. Some of the sensory input goes directly or via thalamus into the amygdala to be processed instantly. This is associated with more primitive, fast and reactive responses to the stimulus, called “Low Road”. Amygdala has close connection with hippocampus which is responsible for our memory and therefore could process these sensory input with the existing memory or create a memory from this new event. Some of the sensory input from the thalamus goes into the higher cortical regions to be processed and then signals the amygdala to activate the stress response. This pathway is called “high Road”. The front part of our brain called prefrontal region is responsible to regulate these responses. This region has the ability to assess and reappraise the stimulus and influence how the individual respond to the event. In other words the prefrontal region has the capability to evaluate the situation in a more intellectual and cognitive manner and inhibit the more primitive and hyper-excited limbic system by top down control and therefore influence how we perceive the stimulus and regulate the subsequent biological responses. Some studies have demonstrated that high stress stimuli could disrupt the ability of the pre-frontal region to regulate the emotions which eventually could lead to chronic stress-related disorders. These chronic, intense and repetitious stressful conditions would also have the potential to impair the pre-frontal executive function and negatively affect our attention, cognitive flexibility and working memory.
The chronic, continuous or repetitious stress conditions are also associated with medical and psychological disorders, including addictive disorders, obesity, hypertension, cardiovascular disease, autoimmune disorders, cancer, Alzheimer`s disease, major depression, anxiety and post-traumatic stress disorders.
Now that we understand the series of events that happen in our brain and body when facing a stressful situation, we might be able to find the appropriate strategies to better cope with those stressors and minimize their harmful effects. Coping stress strategies are thoughts and actions that are used to manage stressful conditions. Researchers have studied and recommended many coping mechanisms. But let’s talk about some of the strategies that in my opinion could be extremely beneficial to cope with stresses at our workplace in health care system. Here I introduce ten relevant coping mechanisms, mostly based on activating, applying and strengthening our higher cortical region, especially pre-frontal area:
-
Reframe your mindset.
It is extremely clear that having purpose in life makes us stronger in difficult times, allows us to perceive the struggles and stressors as unavoidable challenges to reach our goals and prepares us to withstand the pain of the process. Medical profession gives us meaning and purpose of serving others, relieving their pain and healing their physical problems. Recognizing this value of medical profession, believing that what we do in a daily basis is priceless and achieving this goal would require our intentional engagement with daily challenges and struggles, allows us to perceive those events as less overwhelming and harmful.
-
Command your inner conversation
Every one of us is involved in an inner conversation or dialogue. These inner dialogue continues throughout the day intentionally or involuntarily and it`s usually about unimportant and sometimes negative, or even destructive events or thoughts. We can`t escape of our thoughts and in fact they frequently distract our attention or make us worry and anxious. So let`s take charge and command our inner conversation and take advantage of this function of our brain more positively towards better coping with stressful events and calming down our mind.
I recommend every morning before you enter your workplace, wait and remind yourself of the values and purpose of what you do and why you do it and reset your brain in a positive and more productive state to cope with daily challenges. You can also repeat this reminder whenever you encounter any stressful event during the day or before you face patients or their family members. I also recommend that before falling sleep remind yourself of a few positive events that had happened at your workplace on that specific day. In this manner you have the ability to calm down your brain and achieve a more positive state of mind before you end the day.
-
Pause
Everyone knows when we encounter a difficult situation, taking a few deep breaths would help. Yes, this is called “Pause”. Our brain has this capability to react to the stressful events instantly. But if we able to pause that instant reaction whether with few deep breaths or by our inner dialogue we have the potential to allow our prefrontal region to take over our emotional responses by reappraising the situation and influencing our bodily responses in a more intellectual and cognitive manner. Daily practice of “pause” would allow us to perceive the events and stimuli less stressful and gradually see the world differently.
-
Accept and let go
Some of stressful events or stimuli at our work place or in our health care system are unavoidable and impossible to change. In these situations the best response would be acceptance of what we can’t change. This strategy allows our brain to be less hyper-excitable in regards to those events or conditions, and instead it enables us to focus our attention towards the more achievable goals.
-
Discover and accentuate the positive sides of events
Medical profession in its core is associated with pain and suffering, and physical and psychosocial problems of human beings. However in the heart of every sad story lies a positive one. The idea is not to ignore the negativities, but to acknowledge them and discover the positive aspects of the event and accentuate that view and interpretation. After all the stress is what we perceive from the event. Therefore focusing on the positive sides of events would be associated with less harmful response.
-
Sharing and Storytelling
Telling the stories whether happy or sad and sharing our views and our feelings are always associated with relief of pain and stressful events. Acknowledgment of the kind and compassionate acts and celebration of the humanity in our workplace is another way of coping in difficult times. Sharing our problems, realizing this undeniable fact that we are not alone and others feel the same way and empathizing with others are extremely strong coping strategies.
-
Gratitude
Life, regardless of how you define it, is an incredible gift. Therefore recognizing the beauty and magic of life, the gift of being alive, the ability to create authentic connection with others, the opportunity to serve, solve problems and challenges and at the same time feel content for who we become in this process deserves gratitude. Being grateful is a powerful tool for perceiving the life challenges as less stressful events.
-
Practice the essence of humanity, Compassion, Connection, Care and Kindness
Creating humane and authentic connection with others and practicing the essence of humanity, compassion, care and kindness in our workplace would revolutionize our mind and our vision towards life. It transcends our character in which some of stressful events that previously deemed to be overwhelming, now seem so trivial and insignificant.
-
Practice mindfulness meditation:
Paying attention to our mental and psychological health is essential. Numerous studies have demonstrated our ability to transform our brain, called neuroplasticity. Based on this idea, some researchers have recommended strategies such as mindfulness meditation to improve the function of our brain especially prefrontal region which has the incredible role in regulating our emotions. Daily practice of mindfulness meditation has shown not only to be associated with feeling less stressed but also to handle better and recover faster from stressful conditions.
-
Personal health and wellness
It`s hard to serve, be productive and create experience for other human beings in our health care profession when we feel miserable. So first and foremost we have to work on our personal health and wellness. This approach allows us to strengthen our physical and social resources for coping against the stressful events and stimuli. Healthy nutrition, daily exercise, yoga, adequate sleep and rest, engaging in positive activities, lifetime learning and good relationships with friends and family are fundamental strategies for our physical and social health.
Post your medical stories, life stories, nurses stories, doctor stories or any life stories for FREE, here on our website! Click here to submit your story. Thank you!









2 Comments